An Unlikely Candidate Enters the CKD Pipeline
A medication best known for treating constipation may have opened a new line of attack against chronic kidney disease. In a multicenter Phase II study in Japan, researchers found that lubiprostone helped preserve kidney function in patients with moderate chronic kidney disease, according to the supplied source text. The finding is notable not only because the drug is already in use for another condition, but because it points to a treatment strategy that works through the gut rather than directly through the kidney.
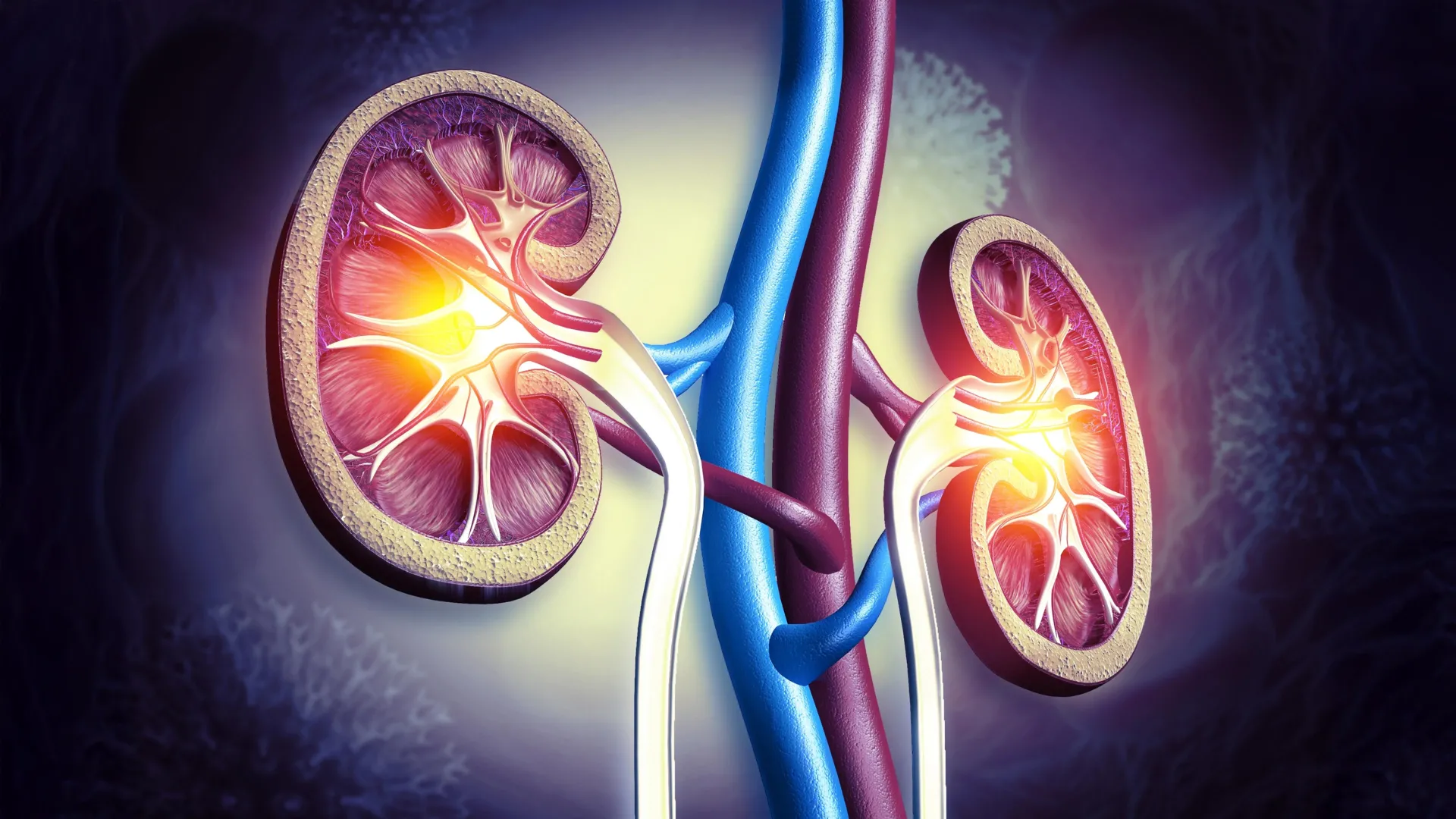
Chronic kidney disease affects hundreds of millions of people worldwide and often progresses slowly until patients require dialysis. Existing therapies can slow deterioration, but the supplied report notes there are still no approved drugs that directly restore kidney function. That leaves clinicians managing decline rather than reversing it. Any intervention that meaningfully preserves function, especially one built on an already familiar medicine, is likely to attract attention.
The trial enrolled 150 patients with moderate CKD across nine medical institutions in Japan. Participants received either lubiprostone or a placebo, allowing researchers to compare how the treatment changed kidney outcomes over time. The result, as described in the source material, was a slower decline in kidney function among those receiving the drug.
The Gut-Kidney Axis Moves Closer to the Clinic
The larger significance of the study lies in the mechanism researchers believe is involved. Doctors and scientists have increasingly focused on what is often called the gut-kidney axis, the relationship between intestinal microbes, inflammation, and kidney health. Patients with CKD frequently experience constipation and disruptions in their gut microbiota. Those changes can contribute to harmful compounds building up in the body, adding stress to already vulnerable kidneys.
The researchers traced lubiprostone's apparent benefit to changes in gut bacteria that increased production of spermidine, a compound associated in the supplied report with healthier mitochondria and reduced kidney damage. That pathway matters because it suggests the drug may be doing more than relieving a symptom. It may be altering a biological environment that helps drive disease progression.
This is a more ambitious proposition than symptom control. It reframes constipation in CKD not just as a discomfort to be managed, but as part of a wider physiological loop that may influence kidney decline. The research team said that idea emerged from observing how often constipation accompanies CKD and then asking whether treating it could improve kidney outcomes rather than merely patient comfort.
Why the Findings Matter Now
The appeal of this result is partly practical. Drug development for chronic diseases is expensive and slow, and kidney medicine has seen fewer breakthroughs than many other fields. Repurposing an existing drug can shorten the path to larger studies if the signal is real. Lubiprostone already has an established clinical use, which may lower some barriers to follow-up work compared with a completely new compound.
Still, the supplied evidence supports caution as much as excitement. This was a Phase II trial involving 150 patients, not a definitive late-stage study. The report describes the findings as promising, but not practice-changing on their own. The next step is to determine whether the protective effect holds up in larger and more diverse populations and whether the biological explanation remains consistent under broader testing.
Several details from the supplied report help explain why the study is attracting interest:
- The trial was placebo-controlled and conducted across nine institutions.
- It focused on patients with moderate chronic kidney disease, a group where slowing decline can materially delay more serious outcomes.
- Researchers linked the effect to microbiome changes and increased spermidine production rather than to a purely symptomatic benefit.
If those findings are replicated, the study could help push kidney medicine toward a more systems-based view of disease, one that includes intestinal health, microbial balance, and mitochondrial function as part of the treatment picture. For patients, the immediate takeaway is more restrained: a familiar drug has produced an unfamiliar result, and that result is strong enough to justify serious follow-up. In a field that still lacks many options to preserve kidney function directly, that alone makes this trial important.
This article is based on reporting by Science Daily. Read the original article.
Originally published on sciencedaily.com