A Late-Stage Pancreatic Cancer Trial Posts a Survival Gain
A randomized phase 2 study published in Nature Medicine reports that adding elraglusib to gemcitabine plus nab-paclitaxel improved survival for patients with previously untreated metastatic pancreatic ductal adenocarcinoma, one of the deadliest solid tumors and one where treatment progress has been limited.
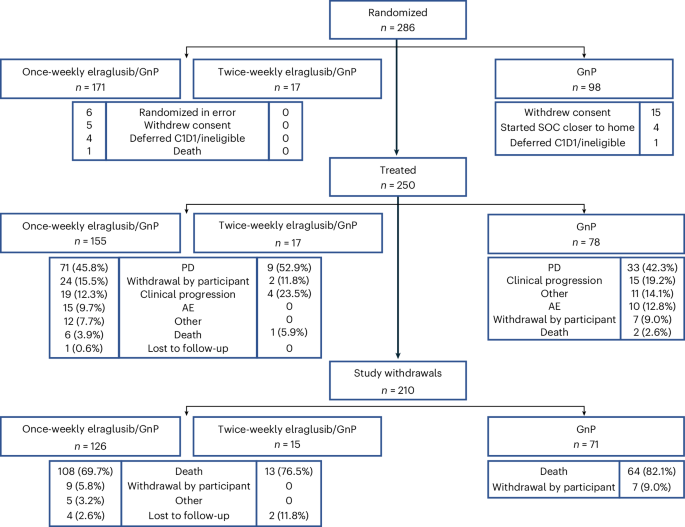
The trial enrolled patients in an open-label, international, multicenter study and randomized them 2:1 to receive either weekly elraglusib with gemcitabine plus nab-paclitaxel or chemotherapy alone. In the prespecified modified intention-to-treat population, 155 patients received the elraglusib combination and 78 received standard chemotherapy.
What the Trial Found
According to the published abstract, the combination improved median overall survival to 10.1 months, compared with 7.2 months for chemotherapy alone. That translated to a 38% lower risk of death, with a hazard ratio of 0.62 and a reported P value of 0.01.
The one-year survival rate also separated meaningfully between the two groups. Patients receiving elraglusib plus chemotherapy reached a one-year survival rate of 44.1%, versus 22.3% in the chemotherapy-only arm.
For metastatic pancreatic cancer, where even modest gains can matter clinically, those numbers stand out. A 2.9-month improvement in median overall survival does not change the seriousness of the diagnosis, but it does suggest that the drug may be doing more than producing a marginal signal.
Why Elraglusib Is Different
Elraglusib, also known as 9-ING-41, is described in the paper as a cell-permeable ATP-competitive inhibitor of GSK-3β. The authors point to a multimodal mechanism of action and prior antitumor activity in preclinical cancer models, including pancreatic cancer.
The trial also included exploratory correlative analyses that may help explain why the regimen worked in some patients. Baseline circulating immune-related factors, including CXCL2 and TRAIL ligands, were associated with improved survival in the elraglusib arm. The investigators also reported increases in intratumoral cytotoxic immune cell populations during treatment.
Those findings do not establish a definitive biomarker strategy yet, but they suggest the drug’s effects may extend beyond direct tumor inhibition and into changes in the tumor immune environment.
Safety Profile Remains a Central Question
The study reported a manageable safety profile, but the added drug came with tradeoffs. The most common grade 3 or higher treatment-emergent adverse events in the elraglusib arm were neutropenia, seen in 52.3% of patients, anemia in 25.2%, and fatigue in 16.8%.
In the chemotherapy-alone arm, the corresponding rates were 30.8% for neutropenia, 29.5% for anemia, and 5.1% for fatigue. That pattern suggests the combination did not introduce unexpected toxicity categories, but it did increase the burden of some serious side effects, especially neutropenia and fatigue.
That balance matters in pancreatic cancer, where patients often have limited functional reserve and clinicians weigh every survival gain against treatment tolerability.
What Comes Next
The authors conclude that the results support the clinical activity of elraglusib plus gemcitabine and nab-paclitaxel as a first-line treatment approach in metastatic pancreatic ductal adenocarcinoma. On the basis of the abstract alone, the study appears to provide one of the clearer late-stage positive signals for a new combination in this disease in recent years.
The next step is straightforward: confirmatory testing. Phase 2 results can shift expectations, but they do not settle clinical practice on their own. A larger trial will be needed to determine whether the survival benefit holds, whether biomarker signals can be used prospectively, and how broadly the regimen fits into first-line treatment decisions.
For now, the study offers a notable development in a field that rarely produces easy optimism. In metastatic pancreatic cancer, a therapy that extends survival while remaining clinically manageable is enough to command attention.
This article is based on reporting by Nature Medicine. Read the original article.
Originally published on nature.com