A systems-level look at a basic human rhythm
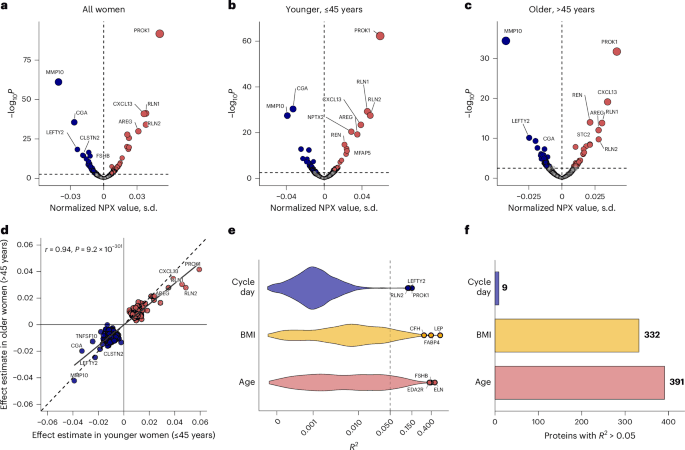
Researchers have produced one of the largest molecular maps yet of how the menstrual cycle reshapes the human body, using blood samples from 2,760 women in the UK Biobank to profile nearly 3,000 circulating plasma proteins. The study, published in Nature Medicine on April 13, 2026, identified 198 proteins that change across the cycle and organize into distinct temporal patterns aligned with menstrual phases.
The work addresses a longstanding gap in medicine. The menstrual cycle is one of the most fundamental recurring processes in human physiology, but many of its system-wide molecular changes have remained poorly described. By examining plasma proteins at scale, the authors aimed to move beyond a narrow hormone-focused picture and build a broader atlas of biological variation across the cycle.
That matters for both research and clinical practice. If many blood-borne molecules rise and fall with cycle timing, then studies that ignore menstrual phase can miss real biology or misread normal variation as disease-related change. A clearer map could also improve the search for biomarkers in women’s health, particularly in conditions where symptoms and tissue biology are shaped by cyclical processes.
What the researchers found
The headline result is the breadth of the proteomic shift. Out of the nearly 3,000 proteins measured, 198 varied across the menstrual cycle. According to the paper’s abstract, those proteins included reproductive hormones, cytokines, and growth factors. The patterns were not random. Instead, they clustered into temporal signatures that matched different phases of the cycle.
The study also found evidence that many of the varying proteins are biologically specific to reproductive tissues. The authors report enrichment in endometrial tissue and expression in epithelial and stromal cell types. That points to a mechanistic link between changing uterine biology and measurable protein signals in blood.
In practical terms, the work suggests the menstrual cycle leaves a detectable fingerprint in the circulating proteome. Blood does not simply reflect a handful of changing hormone levels. It carries a broader, phase-dependent molecular pattern that appears to track coordinated activity across tissues involved in reproduction and immune signaling.
Why this could matter for diagnosis and research design
The authors connected several of the cycle-varying proteins to common reproductive disorders, including endometriosis, leiomyoma, and abnormal bleeding. The source text does not claim that these proteins are validated diagnostic markers for those diseases, but it does show that the cycle-linked signals overlap with conditions that are common, burdensome, and often difficult to characterize.
That overlap is potentially important for two reasons. First, it may help explain why biomarker discovery in women’s health has been difficult when menstrual timing is not carefully accounted for. A protein associated with disease in one setting might also be a normal marker of cycle phase in another. Second, understanding which proteins normally fluctuate could help researchers distinguish background physiology from abnormal biology.
The study therefore adds weight to an argument that has been building across biomedical research: sex-specific and cycle-aware measurement strategies are not optional refinements, but central design requirements for accurate interpretation.
A 75-protein score for cycle phase
Beyond descriptive mapping, the researchers also built a predictive tool. They report developing a proteomic score based on 75 proteins that accurately predicts menstrual cycle phase. The source text does not provide full performance metrics in the excerpt supplied here, so the strongest supported conclusion is that the score was able to classify phase with high accuracy within the study framework.
That kind of score could prove useful in several settings. In research, it may offer a way to infer or confirm cycle phase when self-reported timing is incomplete. In translational work, it could help standardize specimen collection or improve interpretation of blood-based tests that are influenced by reproductive state. It also reinforces the core finding of the paper: the cycle’s molecular signal is robust enough to be detected from a multi-protein blood signature.
Still, a predictive score is not the same as a routine clinical test. Additional validation, including performance across populations and care settings, would be needed before any broader use. The present study is best understood as a foundational resource and proof of principle.
What this changes in the bigger picture
Women’s health research has often been constrained by undermeasurement, fragmented datasets, and a tendency to treat cyclical biology as noise rather than signal. This paper pushes in the opposite direction. It frames the menstrual cycle as a structured molecular program that can be observed at scale and quantified with modern proteomics.
That is likely to influence several adjacent areas. Biomarker studies may need tighter control for menstrual phase. Population studies may revisit prior findings where cycle timing was unavailable. Drug development programs focused on reproductive disorders could gain a richer set of candidate proteins to investigate. And clinical researchers may increasingly view plasma proteomics as a tool for connecting symptoms, tissue biology, and systemic signals.
The resource also has a basic science value. By identifying proteins linked to different phases, and showing enrichment in relevant tissues and cell types, it provides a map that others can use to ask more specific questions about regulation, timing, and disease mechanisms.
The immediate takeaway
The most important outcome is not a single biomarker. It is the demonstration that the menstrual cycle is accompanied by widespread, organized, and measurable changes in the circulating proteome. In a cohort of 2,760 women, nearly 200 proteins moved with cycle timing, several were linked to reproductive disorders, and a 75-protein score could predict menstrual phase.
That combination makes the study notable: it is broad enough to serve as a reference atlas, specific enough to point toward disease-relevant biology, and practical enough to suggest future diagnostic and research tools. For a field that has often lacked systems-level datasets, this is a substantial addition.
This article is based on reporting by Nature Medicine. Read the original article.