A broader look at a fragmented field
Psychedelic research has moved quickly from the margins toward mainstream neuroscience and psychiatry, but one problem has persisted: different imaging studies often point in different directions. Small samples, different scanning methods, and different analysis pipelines have made it hard to tell which findings reflect a true biological signal and which are artifacts of how individual studies were run.
A new paper in Nature Medicine attempts to reduce that uncertainty by combining data rather than adding another isolated experiment. Researchers brought together 11 independent resting-state functional MRI datasets spanning five psychedelic substances: psilocybin, LSD, mescaline, DMT, and ayahuasca. The data came from research groups across three continents and five countries, then were processed through a common analysis pipeline and evaluated with a Bayesian hierarchical model.
The result is one of the largest coordinated looks yet at how acute psychedelic states alter brain function. Instead of presenting a drug-by-drug story, the study searched for common network-level effects that appear across compounds and across sites. That matters because psychedelics are increasingly being studied as potential tools in mental health treatment, yet the field still lacks a firm account of the neural mechanisms that unite these experiences.
A common connectivity pattern emerges
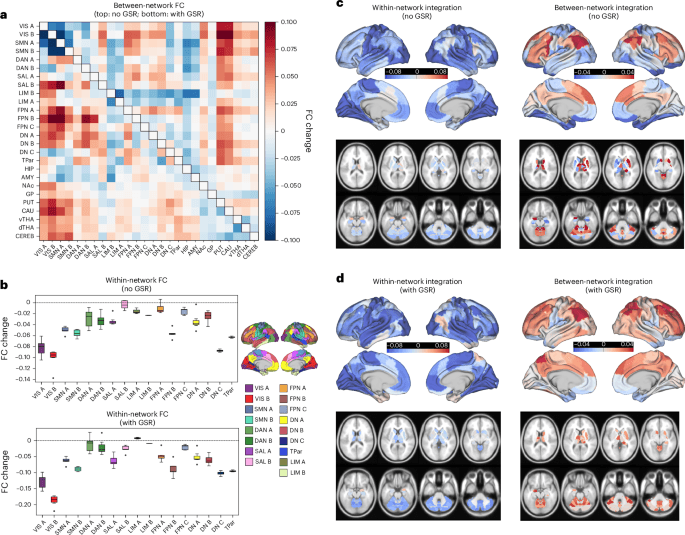
The strongest shared finding was a rise in functional connectivity between transmodal brain systems and unimodal systems. In practical terms, networks associated with internally oriented thought, higher-order control, and emotion-related processing became more connected with networks tied to vision and movement. The paper specifically identifies the default, frontoparietal, and limbic networks on one side, and visual and somatomotor networks on the other.
That pattern fits a long-running idea in psychedelic science: the boundary between high-level interpretation and incoming sensory or bodily information may become less rigid during the acute drug state. The new study does not claim to fully explain the subjective effects of psychedelics, but it does provide evidence that several chemically distinct drugs converge on a related large-scale reorganization of brain communication.
The authors also report that this effect was not completely diffuse. It showed subnetwork specificity, suggesting the changes are structured rather than simply reflecting a brain-wide increase in noise. That is important for a field that has sometimes struggled against the assumption that psychedelics merely produce generalized disruption.
Subcortical and cerebellar changes add depth
The analysis did not stop at the cortex. The researchers found altered involvement in key subcortical regions including the thalamus, caudate, and putamen, along with the cerebellum. Those areas are significant because they sit closer to core functions involving sensory relay, action selection, learning, coordination, and the tuning of broader neural dynamics.
The thalamus in particular has long been central to theories of psychedelic action because it helps gate and route information through the brain. Evidence that thalamic connectivity shifts in a reproducible way across multiple psychedelic compounds adds weight to the idea that these substances alter not just isolated cortical networks but the broader architecture that regulates how information flows.
The inclusion of the cerebellum is also notable. Once treated mainly as a motor structure, the cerebellum is now understood to contribute to cognition and affect as well. Its appearance in a shared psychedelic signature suggests future work may need to examine these drugs as whole-brain modulators rather than tools acting mainly on a small handful of association areas.
Why this matters for clinical research
Psychedelics are being investigated for depression, trauma-related disorders, addiction, and other conditions, yet clinical development has often outrun mechanistic clarity. If researchers can define a robust brain signature that generalizes across drugs, they gain a better foundation for comparing compounds, designing biomarkers, and testing whether certain neural changes track therapeutic response.
This study does not show that the identified connectivity pattern causes clinical benefit, and it does not settle ongoing debates over which psychedelic is best suited to which condition. What it does offer is a more coherent starting point. Instead of a literature built from partially overlapping claims, the field now has a large integrative analysis pointing to a core set of shared effects.
That could also help standardize future work. When multiple labs use different preprocessing choices, even similar raw data can yield different answers. By applying the same pipeline to all 11 datasets, the authors demonstrate how much value there is in harmonization, especially in a field where enthusiasm has sometimes outpaced reproducibility.
The limits remain clear
Even a mega-analysis has constraints. The paper draws from existing resting-state fMRI datasets, so its conclusions are bounded by the quality and design of the original studies. It focuses on acute brain effects rather than long-term change, and resting-state connectivity cannot by itself capture the full complexity of psychedelic experience. Nor does the analysis erase differences among substances, doses, settings, or participants.
Still, the study marks a meaningful advance. Rather than asking whether one small experiment confirms another, it looks for the shared structure inside a scattered body of evidence. For a research area trying to mature into a durable scientific and clinical discipline, that is a significant step.
If the current wave of psychedelic medicine is to rest on something stronger than hype, it will need exactly this kind of cross-site, cross-drug synthesis. The headline finding is not that all psychedelics are identical. It is that, beneath their differences, several of them appear to push the brain toward a recognizable and measurable common state.
This article is based on reporting by Nature Medicine. Read the original article.
Originally published on nature.com