একটি প্রতিরোধযোগ্য সংকট
ক্যান্সারকে প্রায়শই জৈবিক এলাকার একটি কাজ হিসাবে অভিজ্ঞতা করা হয় — একটি পরিবর্তন যা কেউ প্রত্যাশা করতে বা প্রতিরোধ করতে পারে না। একটি ব্যাপক নতুন বিশ্লেষণ সেই ফ্রেমওয়ার্ককে নাটকীয়ভাবে চ্যালেঞ্জ করে। Nature Medicine এ প্রকাশিত গবেষণা দেখায় যে বৈশ্বিক ক্যান্সার বোঝার একটি উল্লেখযোগ্য অংশ ঝুঁকির কারণগুলির জন্য দায়ী যা ব্যক্তি এবং সমাজগুলি পরিবর্তনের ক্ষমতা রাখে: তামাকের ব্যবহার, অতিরিক্ত শরীরের ওজন, অ্যালকোহল খরচ, খাদ্যতালিকাগত ধরণ, শারীরিক নিষ্ক্রিয়তা এবং প্রতিরোধযোগ্য পরিবেশগত কার্সিনোজেনের এক্সপোজার।
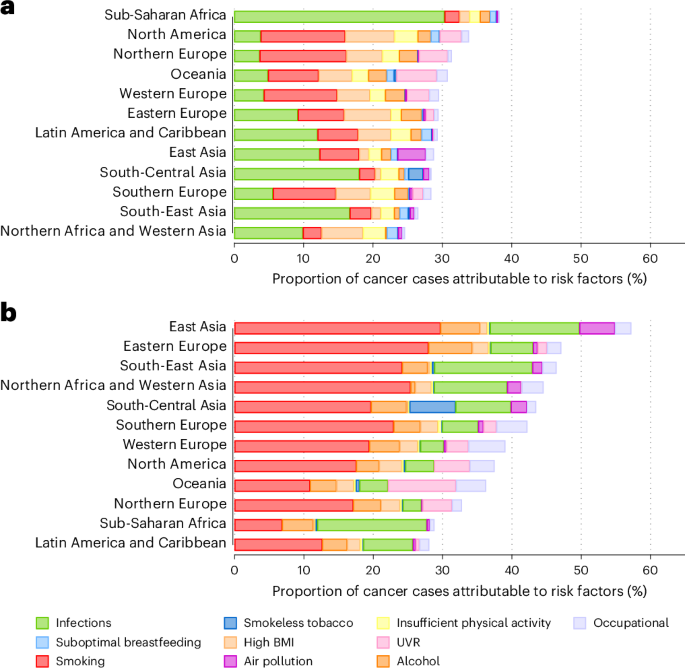
গবেষণায় একাধিক অঞ্চল এবং ডজন ডজন ক্যান্সারের ধরনে ক্যান্সার ঘটনা এবং মৃত্যুর হার সংক্রান্ত ডেটা বিশ্লেষণ করা হয়েছে, যা গবেষকরা ক্যান্সার বোঝার কতটা সম্ভাব্য প্রতিরোধযোগ্য তার সবচেয়ে ব্যাপক হিসাব প্রদান করে — জেনেটিক ভাগ্যের মাধ্যমে নয়, বরং আচরণগত, পরিবেশগত এবং নীতি হস্তক্ষেপের মাধ্যমে যা, নীতিগতভাবে, অর্জনযোগ্য।
নেতৃস্থানীয় পরিবর্তনযোগ্য ঝুঁকির কারণ
তামাকের ব্যবহার উল্লেখযোগ্য মার্জিন দ্বারা একটি একক পরিবর্তনযোগ্য ঝুঁকি কারণ হিসাবে আধিপত্য বজায় রাখে, ফুসফুস, গলা, মুখ, খাদ্যনালি এবং মূত্রথলি ক্যান্সারের অসমতাপূর্ণ ভাগের জন্য দায়ী। দশকের জনস্বাস্থ্য প্রচেষ্টা এবং উচ্চ-আয়ের দেশগুলিতে ধূমপানের হার হ্রাস সত্ত্বেও, তামাকের বৈশ্বিক প্রভাব বিশাল কারণ খরচ নিম্ন- এবং মধ্য-আয়ের দেশের দিকে স্থানান্তরিত হয়েছে যেখানে নিয়ন্ত্রক কাঠামো এবং নিষেধাজ্ঞা সহায়তা কম বিকশিত।
অতিরিক্ত শরীরের ওজন অনেক বিশ্লেষণে দ্বিতীয় সবচেয়ে উল্লেখযোগ্য পরিবর্তনযোগ্য ঝুঁকি কারণ হিসাবে আবির্ভূত হয়েছে এবং এর ভাগ বৃদ্ধি পাচ্ছে। স্থূলতা-সম্পর্কিত ক্যান্সারগুলি এনডোমেট্রিয়াল, স্তন, পেট, কিডনি, লিভার এবং অগ্ন্যাশয় ক্যান্সার অন্তর্ভুক্ত করে। যেহেতু স্থূলতার বৈশ্বিক হার বৃদ্ধি পেয়েছে — খাদ্য ব্যবস্থা পরিবর্তন, আসীন কর্মের ধরণ এবং সামাজিক-অর্থনৈতিক কারণগুলি দ্বারা চালিত যা শক্তি-ঘন খাবারগুলিকে পুষ্টিকর বিকল্পগুলির চেয়ে সস্তা এবং আরও অ্যাক্সেসযোগ্য করে তোলে — তাদের ক্যান্সার ঘটনায় অবদান সেই অনুসারে বৃদ্ধি পেয়েছে।
অ্যালকোহল খরচ, প্রায়শই জনসাধারণের উপলব্ধিতে একটি কার্সিনোজেন হিসাবে অনুমান করা হয়, তৃতীয় প্রধান পরিবর্তনযোগ্য কারণ। লিভার, কোলোরেক্টাম, স্তন, মুখ গহ্বর, ফ্যারিনক্স, ল্যারিনক্স এবং খাদ্যনালি ক্যান্সারের সাথে অ্যালকোহলকে সংযুক্ত করে এমন প্রমাণকে World Cancer Research Fund দ্বারা প্ররোচক হিসাবে চিহ্নিত করা হয়, ডোজ-প্রতিক্রিয়া সম্পর্কের সাথে যা দেখায় ঝুঁকি খরচের প্রতিটি বৃদ্ধির সাথে বৃদ্ধি পায়।
পরিবেশগত এবং পেশাদার এক্সপোজার
স্বতন্ত্র আচরণের বাইরে, বিশ্লেষণ প্রতিরোধযোগ্য পরিবেশগত এক্সপোজারের অবদান পরিমাপ করে: বহিরঙ্গন বায়ু দূষণ, কঠিন জ্বালানি জ্বলন থেকে অভ্যন্তরীণ বায়ু দূষণ, ionizing radiation, ultraviolet radiation এবং পেশাদার carcinogen এক্সপোজার। এই কারণগুলি নিম্ন-আয়ের সেটিংয়ে জনসংখ্যাকে অসমানভাবে প্রভাবিত করে যেখানে শিল্প প্রবিধান, পরিচ্ছন্ন শক্তি অ্যাক্সেস এবং কর্মস্থল সুরক্ষা অবকাঠামো কম বিকশিত — একটি মাত্রা যা ক্যান্সার বোঝার বিশ্লেষণকে একটি তীক্ষ্ণ ন্যায্যতা আয়াম দেয়।
উচ্চ-আয়ের দেশগুলিতে, ট্যানিং বেড ব্যবহার এবং বিনোদনমূলক সূর্যের এক্সপোজার থেকে UV এক্সপোজার মেলানোমা বোঝায় অর্থপূর্ণভাবে অবদান রাখে — একটি ক্যান্সারের ধরন যার ঘটনা ধারাবাহিকভাবে বৃদ্ধি পেয়েছে এমনকি যখন তামাকা-সম্পর্কিত ক্যান্সার হ্রাস পেয়েছে। আচরণগত পরিবর্তনের মাধ্যমে প্রতিরোধের কার্যকারিতা জনসংখ্যা-স্তরের ঝুঁকি কারণ জ্ঞানকে প্রকৃত ঝুঁকি হ্রাসে অনুবাদ করার সম্ভাবনা এবং চ্যালেঞ্জ উভয়ই প্রদর্শন করে।
প্রতিরোধ যা অর্জন করতে পারে
অধ্যয়নের সবচেয়ে উল্লেখযোগ্য অবদান হল সফল প্রতিরোধ কী অর্জন করতে পারে তা পরিমাপ করা। ঝুঁকির কারণ প্রাধান্যের অনুমানগুলিকে ঝুঁকি কারণ-নির্দিষ্ট আপেক্ষিক ঝুঁকি ডেটার সাথে একত্রিত করে, গবেষকরা কেসগুলির ভগ্নাংশকে মডেল করেন যা ঘটবে না যদি প্রতিটি ঝুঁকির কারণকে দূর করা হয়। অনুমানগুলি তাদের স্কেলে ভয়ঙ্করভাবে উত্সাহী: বার্ষিক শত শত হাজার ক্যান্সার-সম্পর্কিত মৃত্যু যা, একটি অর্থপূর্ণ অর্থে, ঐচ্ছিক।
প্রতিরোধ মানে শূন্য ক্যান্সার নয় — জেনেটিক প্রবণতা, অস্পষ্ট জৈবিক বৈচিত্র্য এবং অনিবার্য এক্সপোজার থেকে উত্থিত কেসগুলি সর্বদা থাকবে। তবে প্রতিরোধযোগ্য ভগ্নাংশ এবং যা প্রকৃতপক্ষে প্রতিরোধ করা হচ্ছে তার মধ্যে ব্যবধান বৈশ্বিক জনসংখ্যার স্বাস্থ্যের সবচেয়ে বড় সুযোগগুলির মধ্যে একটি প্রতিনিধিত্ব করে।
নীতি প্রভাব
এই বিশ্লেষণকে নীতিতে অনুবাদ করার জন্য শিল্পগুলির মুখোমুখি হওয়ার প্রয়োজন — তামাকু, অ্যালকোহল, অতি-প্রক্রিয়াকৃত খাদ্য, জীবাশ্ম জ্বালানী — স্থিতাবস্থায় শক্তিশালী আর্থিক স্বার্থ সহ। সবচেয়ে কার্যকর হস্তক্ষেপগুলি পরিচিত: তামাকু কর, বিপণন বিধিনিষেধ, পরিচ্ছন্ন শক্তি রূপান্তর, শহুরে ডিজাইন যা শারীরিক কার্যকলাপ সমর্থন করে, খাদ্য পরিবেশ পরিবর্তন যা পুষ্টিকর বিকল্পগুলিকে আরও অ্যাক্সেসযোগ্য করে তোলে। ঐতিহাসিকভাবে যা অনুপস্থিত ছিল তা জ্ঞান নয় বরং রাজনৈতিক সদিচ্ছা।
Nature Medicine বিশ্লেষণ ক্যান্সার প্রতিরোধকে ক্যান্সার গবেষণা এবং স্বাস্থ্য ব্যবস্থা বিনিয়োগের একটি বড় শেয়ার পেতে হবে এমন যুক্তিগুলির জন্য পরিমাণগত ভিত্তি প্রদান করে যা বর্তমানে পায়। চিকিত্সা গবেষণা তহবিল এবং ক্লিনিক্যাল মনোযোগের বেশিরভাগ দখল করেছে, তবে রোগ বোঝার গণিত পরামর্শ দেয় যে প্রতিরোধ ডলার বাঁচানো জীবনে উল্লেখযোগ্যভাবে বেশি রিটার্ন দিতে পারে।
এই নিবন্ধটি Nature Medicine দ্বারা প্রতিবেদনের উপর ভিত্তি করে। মূল নিবন্ধ পড়ুন.
Originally published on nature.com