A New Frontier in Cancer Treatment
Cancer vaccines occupy a unique position in the history of medicine: a therapeutic concept that has been pursued for over a century but has only recently acquired the biological understanding and technological tools needed to make it work in a clinically meaningful way. A comprehensive review published in Nature Medicine examines where the field stands today, tracing the path from early setbacks to the sophisticated mRNA and neoantigen-targeting approaches now advancing through clinical trials with genuine promise.
The timing of the review reflects genuine acceleration in the field. The mRNA technology platforms that powered COVID-19 vaccines have been adapted for cancer applications with remarkable speed, and early clinical data from personalized cancer vaccine programs has been sufficiently encouraging to attract billions of dollars in investment from pharmaceutical companies that spent years skeptical of cancer vaccination's commercial viability. The landscape in 2026 is fundamentally different from what it was even five years ago.
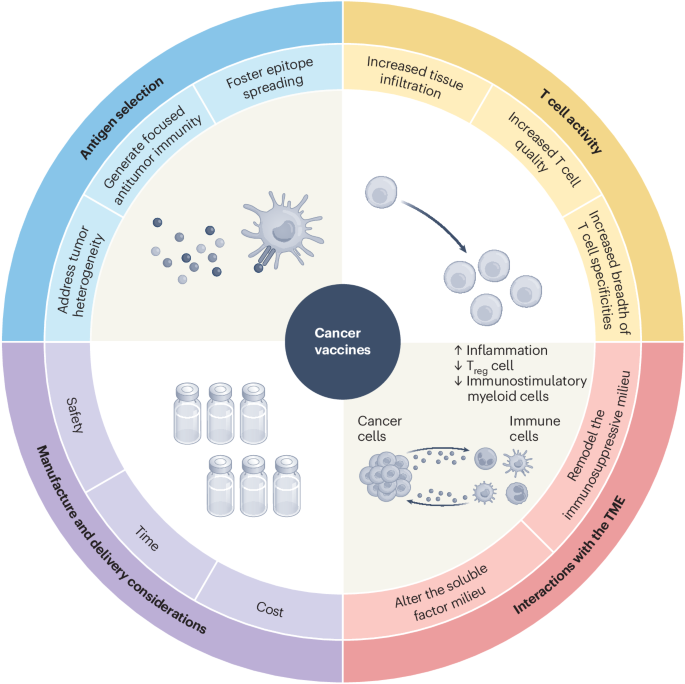
Cancer vaccines work on a different principle than traditional vaccines for infectious disease. Rather than training the immune system to recognize a pathogen before exposure, cancer vaccines aim to train the immune system to recognize and destroy tumor cells that are already present in the body. This therapeutic vaccination approach requires precisely identifying the molecular targets on tumor cells that mark them as foreign and generating an immune response strong enough to overcome the immunosuppressive environment that tumors create to protect themselves from immune clearance.
Personalized mRNA Cancer Vaccines
The most scientifically advanced cancer vaccine approach currently in clinical development uses mRNA technology to create personalized vaccines targeting neoantigens — mutant protein fragments that are unique to an individual patient's tumor. Because these targets are created by the specific mutations in each patient's cancer cells, they are not present on normal tissue, making them highly selective targets for immune attack.
The personalized vaccine development process involves sequencing a patient's tumor to identify its specific mutations, using computational tools to predict which mutant peptides will be displayed on tumor cell surfaces and recognized by immune cells, synthesizing an mRNA vaccine encoding those targets, and administering the vaccine to stimulate an immune response. The entire pipeline, from tumor sequencing to vaccine administration, now takes weeks in advanced manufacturing settings, down from months just a few years ago.
Moderna and Merck have led clinical development in this space with their mRNA-4157 candidate, which in combination with the checkpoint inhibitor pembrolizumab showed a statistically significant reduction in melanoma recurrence in a randomized Phase 2 trial — a result that electrified the field and has been followed by expansion into multiple cancer types. The Nature Medicine review places this result in the context of a broader field that is now evaluating personalized mRNA vaccines across lung, colorectal, bladder, and other cancers.
Shared Antigen Vaccines and Combination Approaches
Not all cancer vaccine programs are personalized. Shared antigen vaccines target protein overexpressed across many patients' tumors — targets like HER2, MAGE, and tumor-associated carbohydrate antigens that are common enough to support off-the-shelf product development with potentially simpler manufacturing and lower cost. These approaches trade some of the specificity of personalized neoantigens for the practical advantages of scalable production and standardized clinical development.
Combination approaches pairing cancer vaccines with checkpoint inhibitors, CAR-T therapies, or other immunotherapy modalities have emerged as a major area of investigation. The rationale is that vaccines prime tumor-specific immune responses while checkpoint inhibitors remove the brakes that tumors use to suppress those responses — potentially producing synergistic anti-tumor activity that neither approach achieves alone. Clinical data from these combinations is accumulating across multiple tumor types.
The review highlights the increasing sophistication of vaccine delivery systems, including lipid nanoparticles optimized for tumor antigen presentation, novel adjuvant formulations that enhance immune activation without excessive toxicity, and in-vivo programmable approaches that generate personalized immune responses using endogenous cellular machinery rather than ex-vivo manufacturing steps.
Challenges and Open Questions
Despite genuine progress, the cancer vaccine field faces significant challenges that the Nature Medicine review addresses directly. Tumor immune evasion — the ability of cancer cells to downregulate antigen expression, create immunosuppressive microenvironments, and develop resistance to immune attack — remains a fundamental obstacle. Vaccines that generate strong initial immune responses may still fail to produce durable tumor control if the tumor evolves to evade the immune response they stimulate.
Patient selection remains imperfectly understood. Some tumor types and some patients appear to respond dramatically to cancer vaccine approaches, while others show minimal benefit, and the biological predictors of response are not yet well enough characterized to guide treatment decisions with confidence. Identifying biomarkers that predict vaccine response is a major research priority across the field.
Manufacturing cost and complexity, particularly for personalized vaccines, remains a barrier to broad access. The process of sequencing a tumor, identifying targets, designing and synthesizing an individualized vaccine, and administering it within a clinically meaningful timeframe involves substantial infrastructure and remains expensive. Bringing these costs down through process innovation and manufacturing scale will be necessary for personalized cancer vaccines to reach their full potential patient population.
The Path Forward
The Nature Medicine review concludes with measured optimism about the trajectory of the field. Several Phase 3 trials are now underway for cancer vaccine candidates in settings where Phase 2 data has been sufficiently compelling to justify the investment. Results from these larger trials will arrive over the next several years and will substantially determine how quickly cancer vaccines move from experimental to standard-of-care treatment in oncology practice.
The convergence of mRNA platform technology, AI-powered neoantigen prediction, rapid tumor sequencing, and increasingly sophisticated understanding of tumor immunology has created the enabling conditions for cancer vaccination to succeed in ways that previous generations of researchers could not achieve. Whether the field will ultimately deliver on the promise of turning the immune system into a broadly applicable cancer treatment remains to be seen, but the clinical evidence is now strong enough to take that possibility seriously.
This article is based on reporting by Nature Medicine. Read the original article.