The Underutilized Medicine
Physical activity is among the most thoroughly studied and consistently validated health interventions available to humanity. Its benefits extend across nearly every major chronic disease category — cardiovascular disease, type 2 diabetes, several cancers, depression, cognitive decline, musculoskeletal disorders, and all-cause mortality. Its cost is minimal. Its side effects are overwhelmingly positive. And yet it remains dramatically underutilized as a public health intervention, with global physical inactivity rates either stagnant or rising in most regions.
A perspective published in Nature Medicine argues that the core problem is not a lack of evidence but a failure of framing and implementation. Physical activity has been treated primarily as a matter of individual lifestyle choice — a recommendation from a doctor, a gym membership, a New Year's resolution — rather than as a population-level intervention deserving the infrastructure investment, behavioral science support, and policy attention we devote to other proven health interventions like vaccination or smoking cessation.
The Evidence Base
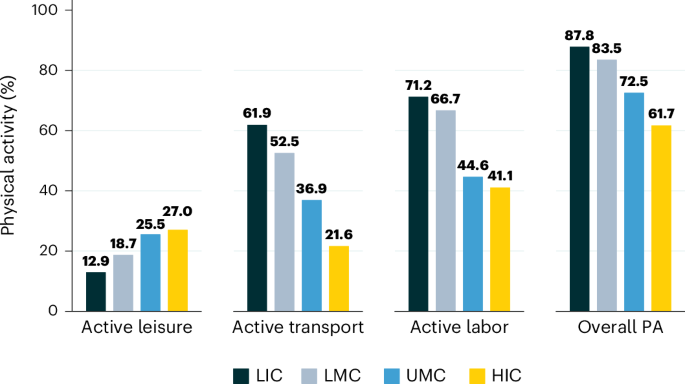
The epidemiological evidence linking physical inactivity to chronic disease is now so robust that it has moved from association to near-certain causality. Prospective cohort studies following millions of people over decades consistently find that those meeting physical activity guidelines — roughly 150 minutes of moderate-intensity activity weekly, or equivalent — experience dramatically lower rates of cardiovascular disease, type 2 diabetes, and all-cause mortality than inactive peers.
The dose-response relationship is well-characterized: even small increases in activity from a sedentary baseline produce substantial health gains, and there is no upper threshold below which increasing activity provides no additional benefit. The evidence is particularly strong for mental health outcomes, with regular physical activity demonstrating efficacy comparable to antidepressant medication for mild to moderate depression in several clinical trials — at zero pharmacological cost and with uniquely positive side effects.